- Services
- Patients & Visitors
- For Healthcare Providers
- Research
- Contact
- Pay My Bill
- Careers
- Donate
- My Health Record
- +1 (401) 227-3669
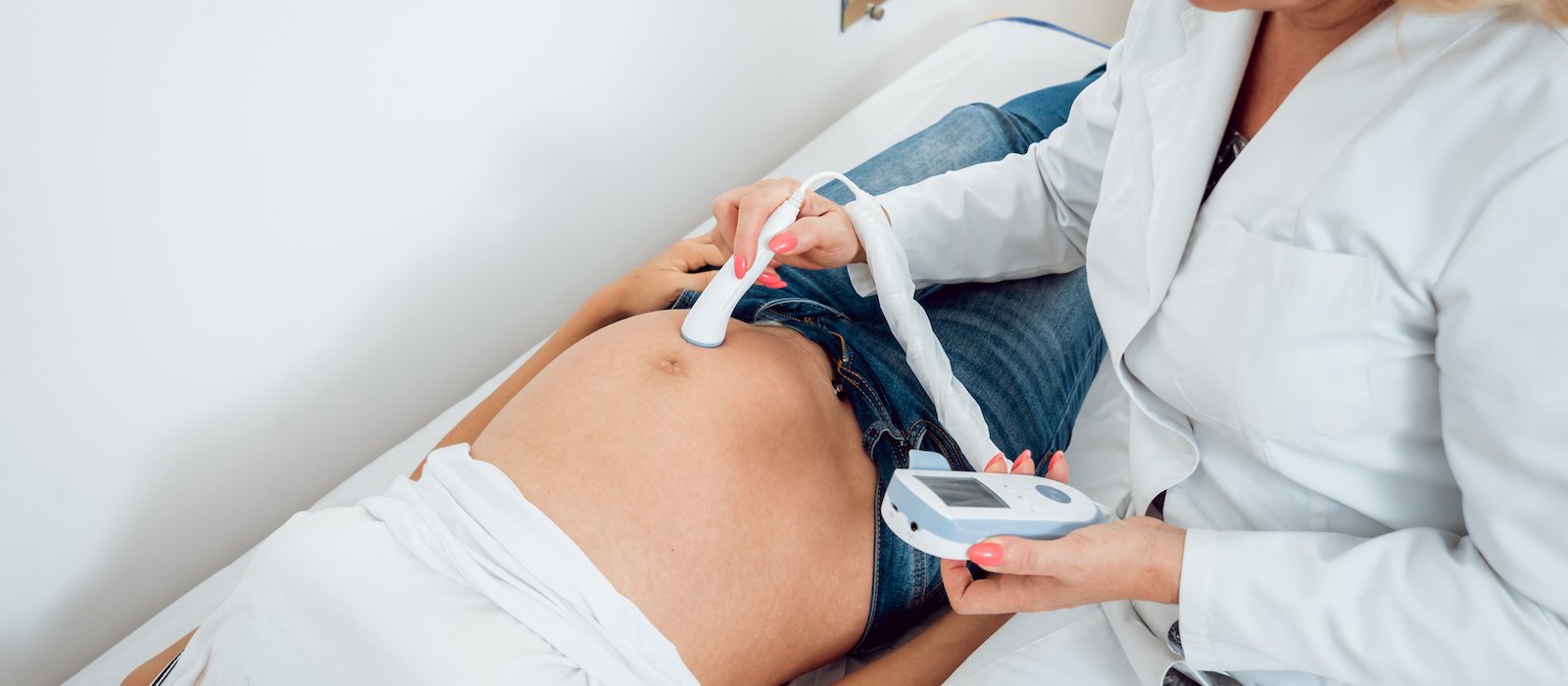
Women & Infants Hospital is a tertiary care center serving Southeast New England. There are 9,000+ deliveries per year. The Division of Maternal Fetal Medicine manages an average of 750 antenatal admissions, provides 500+ consults (inpatient and outpatient) for regional practitioners per year, and performs over 13,000 imaging studies annually. The Prenatal Diagnosis Center supports genetic counseling and outpatient antenatal diagnostic services. Over 6,000 patients receive care annually at this center.
Division of Maternal-Fetal Medicine
Women & Infants Hospital
101 Dudley Street
Providence, RI 02905-2401
P. (401) 274-1100 ext: 47467
F. (401) 453-7622
Fellowship Program Coordinator
Tiffany Le
TLe@Wihri.org
Fellowship Director
Stephanie Ros Saposnik, MD
Srossaposnik@Wihri.org
ABOG eligibility and state medical license
PGY 5-7 equivalent
Fellows devote 15 months of their fellowship learning the clinical skills required of an MFM sub-specialist. Their training is guided by the MFM faculty. This experience provides our fellows an opportunity to become technically skilled, superbly trained sub-specialists and consultants. This clinical exposure is balanced by an intellectual atmosphere consisting of a formal MFM didactic series, together with regular perinatal, genetics and pathology conferences, as well as coursework opportunities.
The Maternal-Fetal Medicine (MFM) Fellowship Program at Women & Infants is designed to provide an in-depth experience in both clinical medicine and research. As the major obstetric referral center for the region, the hospital consults with obstetric patients having a wide variety of clinical problems. MFM specialists also provide both consultative and comprehensive care throughout pregnancy for patients with chronic medical problems and fetal anomalies requiring specialized care.
The research resources available to the fellow are similarly impressive, and fellows devote 14 of their 36 months with us to developing an expertise in clinical and/or basic investigation. The research infrastructure at Women & Infants is currently supported by two large Federal Grants and several foundational grants:
Available grants provide support for development of junior faculty as well as for basic infrastructure. Our affiliation with Brown University and Rhode Island Hospital provides additional research support and possibilities for interdisciplinary research. The MFM division participates in the Maternal Fetal Medicine Units Network sponsored by the NICHD. The research interests of our faculty include:
Research interests outside the expertise of the Division are also fostered, with the collaborative efforts of anesthesiology, neonatology, and pathology producing an outstanding opportunity.
The large clinical volume at Women & Infants allows access to an ample number of potential study patients to support clinical research, addressing both common and uncommon problems. Our close relationship with Rhode Island Hospital and The Warren Alpert Medical School of Brown University also provides many opportunities to collaborate with established researchers doing clinical, translational, and basic science research. Because Women & Infants is a sub-specialty hospital providing female and neonatal health care, there is a close working relationship among all the divisions, which also fosters collaboration.
The Edward Cardillo Health Sciences Library, situated on the third floor at Women & Infants, provides free access to a host of electronic databases for literature search and retrieval. The hospital's affiliation with Rhode Island Hospital and Brown University provides access to more than 3,000 electronic online journals and older periodicals. Journals are available through links to other libraries and university facilities. Access to these databases is available from individual offices and through networked computers.
Brown offers individualized training for fellows and faculty on the use of scientific informatics' resources. The library staff provides reference retrieval services, such as inter-library loan, for obscure or out-of-date publications and books. The library also has computer workstations, scanners, and copy machines. Additional learning opportunities are provided through numerous electronic teaching and educational resources.
Basic and translational research is performed at the hospital's Kilguss Research Institute, a 30,000-square foot wet laboratory, multi-user facility in the Jewelry District. Investigators use this facility to address specific research questions in reproductive biology and women's health. Investigators have access to core facilities and equipment, including:
The Division of Maternal-Fetal Medicine has approximately 1,000 square feet of wet lab space dedicated to basic and translational research. The investigators at Kilguss are currently studying problems such as:
Animals are housed in a neighboring facility operated by Rhode Island Hospital. The Jewelry District houses core research laboratory facilities for Brown University, Rhode Island Hospital and Women & Infants, allowing for the pooling of resources. Each of these facilities is within one to two blocks of each other, providing access to specialized equipment for genetic, proteomic, and structural analysis.
The Division of Maternal-Fetal Medicine is an active member of the Maternal Fetal Medicine Units Network sponsored by the NICHD, through which it participates in various clinical trials related to improving pregnancy outcomes. As a member institution, many of the MFMU resources are available to fellows seeking to answer research questions. The Division is also a member of the National Normal Fetal Growth Study (NFGS), and has participated in a variety of multicenter trials, including the international Hyperglycemia and Adverse Pregnancy Outcome (HAPO) study and the FASTER trial evaluating the use of ultrasound and serum screening for the detection of Trisomy 21. The Division was also a participant in the Stillbirth Collaborative Research Network.
The Department of Obstetrics and Gynecology at Women & Infants has received institutional awards to assist in collaborative research and faculty development. The COBRE award in reproductive biology (NIH) provides infrastructure and salary support for translational and basic research projects. This award is also used to provide salary support for individual investigators early in their career. The Department and Brown have been designated a Center of Excellence in Women's Health. One of the goals of this award is to develop interdisciplinary research directed at improving women's health. For example, this program provides financial support for educational programs and small pilot projects designed to achieve that goal.
The WRHR (Women's Reproductive Health Research) program, sponsored by the NIH, is designed to help obstetricians develop into competitive investigators. The award provides salary support, protected research time, and financial research support for up to three junior faculty members trained in obstetrics and gynecology. This program is ideal for sub-specialty trained individuals who wish to continue research program development during the early phases of their career. The Department's Research Division provides statistical support and consulting for individuals interested in running clinical trials by helping with research design and providing space for seeing and evaluating enrolled patients.
Women & Infants is an affiliate and teaching hospital for Brown University and its Warren Alpert Medical School. We are involved in medical education at multiple levels through the university and support many of the research facilities at Brown and our neighboring Rhode Island Hospital. The affiliation provides easy access to the basic sciences and other clinical sciences in medicine. Brown is located within one mile of the hospital campus, providing easy access to other departments such as engineering, history, and community health.
The Labor and Delivery Suite is located on the second floor of the hospital and has 20 labor/delivery/recovery rooms. In addition, there is an alternative birthing center for low-risk deliveries. The hospital operating rooms are adjacent and three operating rooms are dedicated to obstetrics. All rooms are equipped with central fetal monitors. The unit has 24-hour anesthesia coverage and the ability for invasive monitoring. Portable ultrasound machines are available on the unit with color and pulsed Doppler capability. Patients with Invasive monitoring can be followed in the post-anesthesia care unit, the acute monitoring service, or in the Intensive Care Units at Rhode Island Hospital which is physically connected to Women & Infants.
The Antepartum unit is located in the South Pavilion on the 4th floor. All rooms are single rooms. The unit is equipped with fetal monitors so that NST's can be performed at the bedside. Portable ultrasound machines are available on the unit. Detailed ultrasound exams are supervised by the MFM faculty using state of the art equipment. Invasive fetal procedures are performed in the operating rooms with trained personnel. The fetal surgery program operates in conjunction with the pediatric surgery program centered at Rhode Island Hospital.
The Maternal-Fetal Medicine Service provides antenatal care for high-risk pregnancies at the Obstetrics and Gynecology Care Center on the fifth floor of the Outpatient Medical Facility, 2 Dudley Street. Clinics occur on various half days throughout the week. The clinic is staffed by diabetic nurse educators, nutritionists, social workers, and perinatal nurses. A portable ultrasound unit is available for use to practitioners. Blood drawing, obstetrical ultrasound, and antenatal testing facilities are also located immediately adjacent to our outpatient offices.
The Prenatal Diagnosis Center is a comprehensive center run by the Maternal-Fetal Medicine division that performs prenatal diagnosis via complex ultrasound exams, Doppler, fetal echocardiography, amniocentesis, and chorionic villus sampling, and also provides genetic counseling and fetal testing. This targeted ultrasound facility is equipped with GE Voluson E8 machines, and is staffed by RDMS certified technologists. This unit also has trained perinatal nurses who perform NSTs, amniotic fluid assessments, and biophysical profiles. Trained genetic counselors are available five days a week and provide counseling by appointment or on an urgent basis when necessary. Counselors provide follow-up and referral services when needed. The Prenatal Diagnosis Center is open five days per week. The Maternal-Fetal Medicine Division also provides prenatal diagnosis and consultative services at multiple offsite facilities in Rhode Island (Wakefield) and Massachusetts (North Dartmouth, New Bedford, Fall River, and Wareham).
The three-year fellowship is structured as an integrated experience. The time is focused on specific areas of Maternal-Fetal Medicine (MFM) including inpatient care, ambulatory consultation, prenatal diagnosis, reproductive genetics, and research. During each year, the fellow will spend approximately 6-8 months dedicated to (1) learning ultrasound and prenatal diagnosis, (2) running the inpatient high-risk, or (3) participating in outpatient MFM and Reproductive Genetics consultations. The remaining 4-6 months are committed to research and didactics. Each fellow spends a half-day of every week in the Obstetrics and Gynecology Care Center providing antenatal care to women with high-risk pregnancies. Fellows share night call responsibility with the MFM faculty taking an average of 3-4 night calls a month in which they are responsible for transports, emergency consultations, and the MFM inpatient service.
The fellows are supervised by the MFM faculty throughout their fellowship. An MFM faculty member provides supervision of antenatal care. The fellow is assigned an MFM backup attending while covering the inpatient service or consultation service. Laboring patients are managed by the individual assigned to the inpatient service with the MFM attending backup when a fellow is covering. Prenatal diagnosis training is supervised by one of the MFM faculty members assigned to the Prenatal Diagnosis Center (PDC). An MFM attending is assigned as a backup when fellows are covering night calls. Research project supervision is provided by the research mentor as well as by the research faculty within the Division.
Fellows are not required to take additional graduate-level courses to complete their fellowship. Graduate-level courses are available through Brown University and support is available within the Division to participate in these. During their MFM fellowship, prior Women and Infants’ fellows have completed course work and earned MPHs, Certificate in Healthcare Quality, and Public Health certificates (through the Hassenfeld Scholars program).
The consultation service provides outpatient consultation to referring providers for:
Consults are reviewed with the backup attending to discuss nuances of management. Fellows provide management recommendations and assist the referring physicians in obtaining necessary diagnostic tests. Consults are provided in a timely manner to the referring physicians after discussion with the backup attending.
The Division provides a continuity clinic to provide prenatal care for MFM patients. The fellows follow their own assigned patients with backup by the MFM attending, based on diagnosis and degree of complication. Patients are distributed to allow for depth and breadth of clinical exposure during the fellowship. Fellows determine and execute management plans for their own patients. All new MFM patients are reviewed at least once at ‘Chart-Flip’ rounds that are held twice monthly.
The Antenatal Office has additional internal resources for patients with pre-gestational and gestational diabetes including nutritionists, diabetes nurse educators, and a perinatal nurse coordinator.
The Division provides diabetes in pregnancy educational programs to patients as a service for referring physicians. These include:
These services are scheduled through the MFM administrative offices.
The Women & Infants' Genetic Counseling Program provides fellows with clinical training in perinatal genetics as supervised by those faculty members trained and board-certified in MFM and Genetics. Fellows will participate in genetic counseling by direct observation of the genetic counseling staff during their prenatal diagnosis rotation. Preconception counseling and pregnancy-related genetic counseling are provided by MFM, MFM-genetics, or genetic counselors, depending on the consultation request. Such consultations frequently include:
Fellows also participate in prenatal care for patients with genetic disorders during their ambulatory rotations. Training to learn CVS is available through the MFM faculty.
The Prenatal and Special Testing Program, under the direction of Geralyn Messerlian, Ph.D., covers the state and is internationally-renowned for developing new serum screening methods. The Division provides genetic counseling and evaluation for both low and high alpha-fetoprotein tests. This facility provides first and second-trimester serum screening as well as many other specialized tests.
The cytogenetic laboratory, under the direction of Umadevi Tantravahi, MD, within the hospital's Department of Laboratory and Pathology Medicine, provides:
Targeted obstetrical ultrasound is provided by the Division of Maternal Fetal Medicine at its PDC, which is a comprehensive counseling, diagnosis, and testing unit. Screening ultrasound examinations are provided in the general community and through the hospital Department of Diagnostic Imaging. The PDC is a referral based practice.
Ultrasound training involves both hands-on acquisition and image review. Training is integrated into clinical rotations and special didactic sessions. Screening fetal echocardiography is performed by MFM. Identified abnormalities are referred to pediatric cardiology for consultation. During this time, fellows are exposed to:
Time is also spent on counseling parents facing newly identified and previously identified abnormalities.
In the first year, the fellow has four-week didactic sessions at the beginning of the year to concentrate on prenatal ultrasound examinations.
Up to 6 months each year is devoted to research and didactic activities (14 months allotted over the course of the fellowship). Research and didactic time is scheduled in blocks of no less than four weeks. Block time is tailored to the individual fellow's project needs. During the research blocks, one-half day a week is spent in the Antenatal Office.
Fellows are encouraged to pursue both clinical and translational research projects during their fellowships. There are available facilities for fellows who chose to pursue basic science research projects. The fellow's research project is determined individually. Fellows are encouraged to design projects that are interdisciplinary within Women & Infants and across the university. A research mentor is selected based on the project focus. Mentors provide:
Fellows are additionally expected to meet with MFM research faculty at the beginning and end of each research block to establish goals and expectations. Senior faculty from the Brown School of Public Health are available to meet with fellows on a regular basis to discuss study design and review research manuscripts.
Fellows are encouraged to apply for internal and external funding for research projects to learn how to develop a research program and learn the grant process. Fellows receive mentorship from both faculty and project advisors.
Fellowship didactic lectures occur weekly. The lectures are focused on advances within MFM as well as outside the field. This program also covers topics such as research design and informatics. Speakers from other subspecialties such as pediatric cardiology, diagnostic imaging, laboratory medicine, immunology, anesthesiology, and genetics present on a regular basis. Fellows are expected to have their own independent study program for basic issues in MFM.
Multidisciplinary Antenatal Diagnosis & Management Conference (MADAM) is an integrated conference focused on antenatal management and post-hoc review of prenatally identified abnormalities. The conference occurs twice a month and involves the participation of:
The conference typically involves three presentations from different disciplines related to specific topic or case. The goal is to provide a multi-disciplinary approach to clinical management, taking into account all related perspectives.
This is a monthly conference coordinated by the COBRE in Perinatal Biology. This is a research conference held at the Kilguss Research Building Institute. It focuses on basic and translational research related to obstetric and neonatal medicine. Presentations are made by local and nationally recognized investigators.
The Women & Infants Maternal Fetal Medicine (MFM) fellowship program accepts applications through the ERAS system. Please refer to the website for application information and other requirements and deadlines.
In order for an application to be considered for review, it must be complete in the ERAS system. The following documents are required to be uploaded with your application to be considered complete:
Application deadline is April 27, 2026. We will start reviewing completed applications on May 1st. All candidates who are selected for an interview will be contacted via email by May 18, 2026. Interviews will be held on July 10, 2026, and July 31, 2026.
The Maternal Fetal Medicine fellowship program is a member of the National Resident Matching Program. The program complies with and follows the guidelines as a member. Applicants must register with the NRMP.
We appreciate your interest in our Maternal Fetal Medicine fellowship program and look forward to receiving your application!
Medical School: University of Virginia School of Medicine
Residency: Thomas Jefferson University Hospital
Fellowship: Women & Infants Hospital/Brown University
Research Interests: Health policy, global health, adolescent health, diabetes in pregnancy, labor management, disability in pregnancy
Fun Fact: I played rugby for Brown during my undergraduate!
Medical School: Women & Infants Hospital/Brown University
Residency: Women & Infants Hospital/Brown University
Fellowship: Women & Infants Hospital/Brown University
Research interests: Medical education, using digital health to improve complex counseling, prenatal genetics
Fun fact: I know the lyrics to most pop songs from the 1940s to now.
Medical School: Florida State University College of Medicine
Residency: Hospital of the University of Pennsylvania
Fellowship: Women & Infants Hospital/Brown University
Research interests: trauma-informed care models in reducing birth trauma among marginalized populations, improvement in patient experience among patients admitted to the antepartum service, global health initiatives, impact of birth trauma on long term health outcomes, reduction in preeclampsia morbidity
Fun fact: I love traveling and have been to every continent except Antarctica!
Medical School: Pacific Northwest University of Health Sciences College of Osteopathic Medicine
Residency: University of Massachusetts Chan Medical School
Fellowship: Women & Infants Hospital/Brown University
Medical School: John Hopkins University School of Medicine
Residency: Northwestern University
Fellowship: Women & Infants Hospital/Brown University
Research Interests: Health equity, immigrant and global health, diabetes and hypertension in pregnancy, mental health, implementation science, medical education.
Fun Fact: I have lived in several places including Spain, Japan, Puerto Rico, and the US! I love photography. Also am a huge dog lover and hope to open a dog rescue one day.
Medical School: Sidney Kimmel Medical College at Thomas Jefferson University
Residency: Women & Infants/ Brown University
Fellowship: Women & Infants/ Brown University
Copyright © 2026 Care New England Health System